Biomedical engineers at the University of Virginia (UVA) and Johns Hopkins University (JHU) have developed a prolific collaboration that has generated several long-term, multi-million-dollar focused ultrasound research grants.
Richard Price, PhD, Research Director of the UVA Focused Ultrasound Center and Justin Hanes, PhD, Director of the Center for Nanomedicine at the Wilmer Eye Institute and JHU School of Medicine, are developing nanoparticles that can be delivered deep into the brain with the assistance of focused ultrasound. Their work has earned them nearly $7 million of National Institutes of Health (NIH) funding from 2011 to 2020 to propel their discoveries to the clinic.
 In their UVA biomedical engineering laboratory, Price and his team (pictured at right) used focused ultrasound to allow the targeted and controlled delivery of nanoparticles deep into the brain. Justin Hanes and his team at JHU are creating the nanoparticles that Price is delivering. These nanoparticles are essentially encapsulated—or coated—molecules, such as chemotherapy drugs or protein-coding nucleic acids (like RNA or DNA).
In their UVA biomedical engineering laboratory, Price and his team (pictured at right) used focused ultrasound to allow the targeted and controlled delivery of nanoparticles deep into the brain. Justin Hanes and his team at JHU are creating the nanoparticles that Price is delivering. These nanoparticles are essentially encapsulated—or coated—molecules, such as chemotherapy drugs or protein-coding nucleic acids (like RNA or DNA).
“With the focused ultrasound technology, virtually anything in the central nervous system that was unreachable before is now possible to access for targeted drug and gene delivery.”—Richard Price, PhD
“This is the perfect melding of two technologies,” says Dr. Hanes. “We are working to deliver powerful, therapeutics non-invasively to targeted diseased areas of the brain. Our goal is to achieve important biological effects while minimizing side effects.”
“We are proud to have supported some of the early validating work conducted by Rich and Justin,” said the Foundation’s Chief Scientific Officer, Jessica Foley, PhD. “Their collaboration is a perfect model for the synergistic potential of focused ultrasound across disciplines and institutions. With these new grants, they will have the resources to quickly translate their research into benefits for patients.”
 A Fundable Model
A Fundable Model
The key to the success of this collaborative and multidisciplinary team is two-fold. First, they have developed a research platform that has produced measurable and critical results in many different disease models, including brain tumors and Parkinson’s. Secondly, they have established multiple collaborative relationships with scientists whose projects and novel therapeutic targets work well on the platform. For example, Price and Hanes are working with neuro-oncologists to more effectively inhibit tumor growth and with immunologists to stimulate and enhance the body’s ability to attack brain metastases.
The Johns Hopkins Contribution
As a leader in nanotechnology medicine, Dr. Hanes invents, designs, and manufactures unique biodegradable plastics to encapsulate molecules, essentially creating the miniscule drug-filled particles that are delivered to specific sites in the body. “The particles move really well through the tissue,” said Dr. Price. “Even after some molecules are introduced, the tissue itself inhibits them from penetrating deeper. The process developed by the Hanes group is innovative and superb because their coating makes the nanoparticles stealthy and able to slide through tissue pores easily.” Products based on Dr. Hanes’ drug delivery inventions have been ed in various clinical trials up to Phase III, and he has founded a few companies to commercialize these inventions.
Project Details
The 2012 NIH/NCI $1.65M grant for the first generation of nanoparticles is expected to be translated into clinical trials within the next few years. The nanoparticles carry FDA-approved drugs that may benefit patients with glioblastoma multiforme (GBM), and the encapsulated drugs are infused directly into the brain following surgery to remove the bulk of the tumor. Safety and effectiveness ing of the nanoparticles administered into the brain by convection-enhanced delivery (an injection with a certain amount of time and pressure) will be studied first, and then focused ultrasound—enhanced delivery will follow.
The therapeutic approach for the NIBIB R01 grant is to overexpress micro RNAs (miRNAs) that inhibit tumor growth. The project collaborators are UVA neuro-oncologists Benjamin W. Purow, MD, and Roger Abounader, MD, PhD, who screened human GBM samples for the miRNAS that regulate tumor growth and used bioinformatics to predict which ones contribute to the growth of the tumor and which ones might suppress it. For these preclinical studies, they will incorporate miRNA targets into specialized nanoparticles and deliver them to the tumor.
For the new NCI grant, the Johns Hopkins team will produce nanoparticles that contain genes that stimulate the body’s immune system (e.g., T cells) to attack brain metastases. The UVA team, led by cancer immunologists Tim Bullock, PhD, and Victor Engelhard, PhD, will use focused ultrasound to deliver these nanoparticles to a model for melanoma that has metastasized to the brain. The researchers’ hope is that the gene delivered directly to the metastatic brain tumor will trigger an immune response. “The potential for this approach is fascinating. The holy grail would be to treat one lesion and have it create a systemic immune response against all of the other metastatic lesions,” said Dr. Price.
 Read an Investigator Profile of Richard Price >
Read an Investigator Profile of Richard Price >
 Read an Investigator Profile of Justin Hanes >
Read an Investigator Profile of Justin Hanes >
—————-
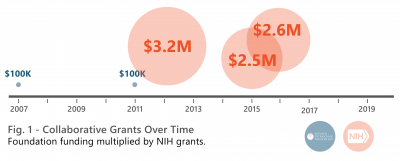
Fig 1. This graphic shows research originally funded by the Foundation and the significantly magnified follow-on funding from NIH.
- 2007-2008 Focused Ultrasound Foundation $100,000 grant for Targeted Delivery of Controlled Release Nanoparticles to Brain Tumors Using Contrast Agent Microbubbles and High-Intensity Focused Ultrasound
- 2011-2013 Focused Ultrasound Foundation $100,000 grant for Delivery of Brain Tumor Penetrating Nanoparticles across the Blood Brain-Barrier with MR-Guided Focused Ultrasound
- 2011-2015 NIH/NCI $3.2M grant for first generation nanoparticle study will be the first to be translated into clinical trials. They carry FDA-approved drugs that may benefit patients with GBM
- May 2015 NIH/NIBIB R01 $2.5M grant for MR-Guided Delivery of miRNA-Bearing Nanoparticles to GBM with Focused Ultrasound
- June 2015-May 2020 NIH/NCI $2.6M grant for MR-Guided Delivery of immunotherapies to brain metastases in a Metastatic Melanoma Model
