 A 15-year-old female diagnosed with a benign brain tumor called a hypothalamic hamartoma (HH) presented to Nicklaus Children’s Hospital in Miami, Florida, in 2019.
A 15-year-old female diagnosed with a benign brain tumor called a hypothalamic hamartoma (HH) presented to Nicklaus Children’s Hospital in Miami, Florida, in 2019.
When the patient was only six months old, her parents noted signs of early puberty, and an MRI of her brain confirmed the diagnosis of a HH. From the age of six months to 12 years, hormonal therapy prevented pubertal progression. Unlike many patients diagnosed with HH, she did not suffer from seizures or mood changes, but struggled with hyperphagia – the abnormally strong desire to eat, often leading to overeating and weight gain. The patient’s parents described her as having a constant appetite: Once she began eating, she never wanted to stop. In the few years prior to her presentation in 2019, she was gaining an average of 18 pounds every six months. She was able to curb some of the weight gain with intense dietary restrictions, but her quality of life as an adolescent was adversely affected.
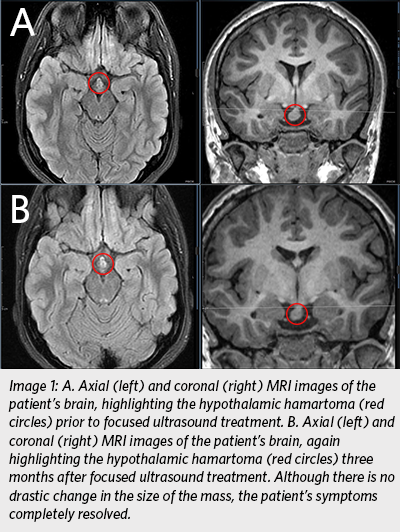
At the hospital visit in 2019, neurosurgeon John Ragheb, MD, and neurologist Ian Miller, MD, determined she was a candidate for a clinical trial using focused ultrasound to treat children with benign brain tumors. An MRI of the patient’s brain clearly indicated a mass protruding from the hypothalamus that was consistent with HH (Image 1A*). On October 16, 2019, the patient underwent focused ultrasound treatment of her HH without adverse effects, and she was discharged from the hospital within 48 hours.
Almost immediately after focused ultrasound treatment, the patient’s hyperphagia symptoms began to disappear. Although follow-up MRI imaging still showed the presence of a mass that was almost unchanged in size (Image 1B), the patient noted a remarkable decrease in her appetite. She has experienced no side effects, and in the six months since the procedure, she has lost 28 pounds (Image 2).
Discussion
Background
HHs are congenital, benign tumors located in the hypothalamus. Centrally located near the base of the brain, the hypothalamus plays a crucial role in many important functions such as releasing hormones and regulating body temperature.
 HHs located in the posterior region of the hypothalamus are associated with medication-resistant epilepsy and cognitive and behavioral dysfunction. HHs located in the anterior region of the hypothalamus are associated with endocrine abnormalities, namely early puberty and obesity, such as with the patient described above.
HHs located in the posterior region of the hypothalamus are associated with medication-resistant epilepsy and cognitive and behavioral dysfunction. HHs located in the anterior region of the hypothalamus are associated with endocrine abnormalities, namely early puberty and obesity, such as with the patient described above.
In patients with medication-resistant hamartoma epilepsy, surgical removal or disconnection of the hamartoma is the treatment. Although open surgery results in good symptom control, there is a high complication rate (up to 30 percent). Less invasive procedures, such as stereotactic radiosurgery by Gamma Knife, laser interstitial thermotherapy (LiTT), and radiofrequency ablation, have proven safer than open surgery for HHs, but these treatments still carry risks and have not been extensively studied. Of note, the goal of most surgical interventions is not to remove the tumor in its entirety, but to “disconnect” the hamartoma cells from the base of the hypothalamus. It is thought that the disconnection of these cells from normal tissue should then result in a loss of the abnormal firing of the brain circuits that lead to seizure activity and the abnormal secretion of hormones.
Focused Ultrasound for HH
Focused ultrasound has the potential to provide a completely noninvasive alternative to other surgical disconnection procedures to treat symptomatic HHs and other centrally located benign brain tumors in children and young adults. The focused ultrasound beams are aimed at the HH using MRI guidance with the goal of thermally ablating the area to “disconnect” it from the surrounding brain circuitry, not necessarily to completely remove the tumor.
Neurosurgeon John Ragheb, MD, of Nicklaus Children’s Hospital in Miami, Florida, is leading a clinical trial with colleagues Ian Miller, MD, and Travis Tierney, MD, to explore the safety and feasibility of focused ultrasound ablation for benign brain tumors requiring surgical intervention in children and young adults. The trial is using Insightec’s Exablate Neuro System.
As evidenced by this case report, focused ultrasound holds promise for the noninvasive treatment of certain pediatric brain tumors, and, in particular, in ameliorating debilitating side effects such as epilepsy and obesity. To date, five patients have participated in the clinical trial, and the investigators seek to enroll an additional five patients to complete enrollment in this safety study.
The study is jointly funded by the Foundation and Nicklaus Children’s Hospital.
For more information regarding this clinical trial and other focused ultrasound brain tumor clinical trials, visit the Foundation’s website: https://www.fusfoundation.org/diseases-and-conditions/neurological/brain-tumors.
Meet the Patient
Madeleine’s story was featured in a blog post for the patient support organization, Hope for Hypothalamic Hamartomas.
*Correction: Image 1A has been updated to reflect the accurate tumor target. The image in the original May 28 newsletter was incorrect.
